Australian Researcher Awarded $100K to Study Non-invasive Ventilation for Sleep-disordered COPD Patients
Australian researcher David Geoffrey Chapman has been awarded $100,000 by the American Thoracic Society (ATS) Foundation and ResMed to investigate how non-invasive ventilation can help improve sleep patterns in patients with chronic obstructive pulmonary disease (COPD) and obstructive sleep apnea (OSA) overlap syndrome.
Dr. Chapman, BSc, PhD, is a Chancellor’s postdoctoral research fellow at the School of Life Sciences of the University of Technology in Sydney, Australia, who has been studying how different factors, such as obesity and tobacco use, may alter lung function and contribute to the development of respiratory diseases, including COPD and asthma.
In OSA, the tongue falls back against the soft palate during sleep, and the soft palate and uvula fall back against the back of the throat, thereby closing the upper airway and interrupting airflow. This results in fragmented sleep, daytime sleepiness, morning headaches, depression, and a general feeling of being unwell. Patients with OSA are at increased risk of developing high blood pressure, heart disease, strokes, and diabetes.
One in four people with COPD also have moderate to severe OSA, according to a 2017 study.
In COPD/OSA overlap syndrome, patients’ struggle to maintain adequate oxygen and carbon dioxide levels is compounded by their lack of restful sleep and the interrupted breathing caused by OSA.
“Chronic obstructive pulmonary disease is one of the leading causes of death in the U.S. and sleep-disordered breathing, which commonly occurs in patients with COPD, has been found to be a risk factor for premature death in this population,” Sanjay Patel, MD, chair of the ATS Assembly on Sleep and Respiratory Neurobiology, in a press release.
“Through ResMed’s support, this new award will provide a much-needed source of funding for scientists such as Dr. Chapman to determine how to best treat sleep-disordered breathing in patients with COPD in order to improve their lives,” Patel added.
ATS believes more research is needed to address the needs of patients with COPD/OSA overlap syndrome, including an improved understanding of the relationship between the two diseases, more precise definitions, and the best therapy options available.
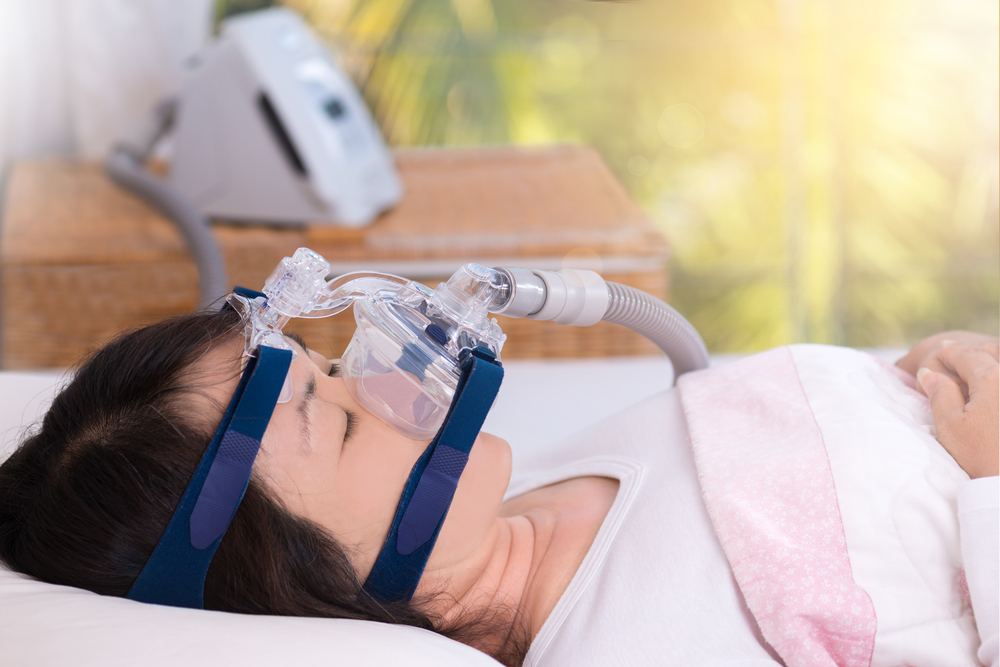
The most common treatment for OSA is positive airway pressure therapy, a form of non-invasive ventilation (NIV) in which a small machine delivers pressurized air through a mask to keep the airway open during sleep.
The new grant will allow Chapman to investigate various NIV settings and their effectiveness in addressing hyperinflation, where trapped air compresses healthier lung tissue and flattens the diaphragm, making it difficult for COPD patients to breathe. A pilot study showed that hyperinflation is correlated with reduced sleep quality.
“ResMed has sponsored rigorous scientific research for decades and is proud to support the ATS Foundation and Dr. Chapman in this important new study,” said Carlos M. Nunez, MD, ResMed’s chief medical officer.
“The more that researchers can confirm how sleep apnea and comorbid conditions interact to affect patients’ health, the more focused and motivated the medical community should be to identify those who are suffering and get them screened, diagnosed, and effectively treated as soon as possible,” Nunez added.






